
Measurable Financial and Operational Benefits
Streamline your claims workflow, reduce errors, and accelerate cash flow with Amuram Consultancy’s end-to-end claims management solutions. Our integrated approach leverages expert teams, AI-driven automation, and proactive oversight, from pre-submission scrubbing to remittance posting—to ensure accurate, timely reimbursements, minimize denials, and optimize revenue cycle performance.
Comprehensive Claims Lifecycle Services
Our comprehensive claims management suite covers every phase of the claim lifecycle to ensure maximum reimbursement and operational efficiency.
- Pre‑Submission Claim Scrubbing
Validate patient demographics, coding accuracy, and payer rules using automated edits and expert review. - Electronic & Paper Claim Submission
Submit claims via HIPAA‑compliant clearinghouses or direct payer portals, ensuring full transparency and audit trails. - Remittance Posting & Reconciliation
Apply electronic remittance advices (ERAs) and paper EOBs, reconcile variances, and maintain precise aging reports. - Denial Prevention & Appeals
Analyze denial drivers, implement corrective action plans, and prepare comprehensive appeal packets to recoup lost revenue. - Patient Payment Coordination
Generate statements, coordinate payment plans, and assist with patient inquiries to close balance gaps.

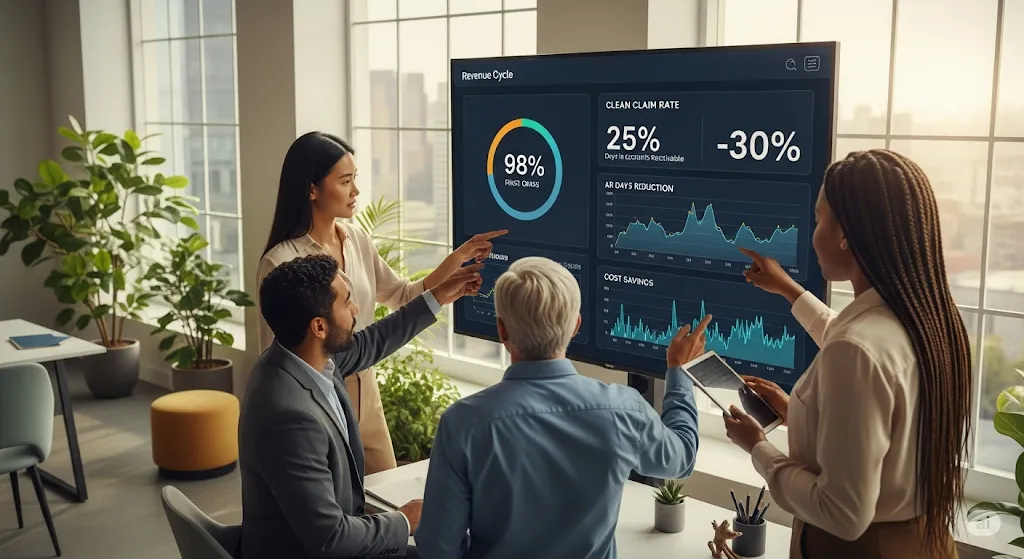
Measurable Financial and Operational Benefits
Leverage clear advantages designed to boost clean-claim rates, expedite payments, and provide strategic insights into your financial performance.
- Higher First‑Pass Acceptance: Achieve a 98%+ clean-claim rate by catching errors before submission.
- Faster Cash Flow: Reduce days in accounts receivable by up to 25% with streamlined processes.
- Cost Savings: Lower operational expenses by up to 30% through automation and flexible staffing.
- Actionable Insights: Gain real‑time visibility into claim statuses, denials, and financial performance via custom dashboards.

Why Partner with Amuram Consultancy?
Process Blueprint
Amuram Consultancy’s proven process blends specialized expertise and cutting-edge technology to deliver a seamless, high-impact partnership that drives measurable results.
Deep Domain Expertise
Certified coders and claims specialists with extensive payer knowledge.
Technology‑Driven
AI‑powered claim edits and automated workflows eliminate manual bottlenecks.
Seamless Integration
Secure API connections to all leading EHR/PM systems for data synchronization.
Dedicated Support
Single point of contact with regular performance reviews and continuous optimization.
Elevate your claims performance and reclaim lost revenue
Begin your journey to streamlined claims and improved cash flow by connecting with our team, your success is just an assessment away.
info@amuramconsultancy.com
Amuram Consultancy Services Private Limited, 16-1A, KLD Road, Anantapur, AP-515004.

